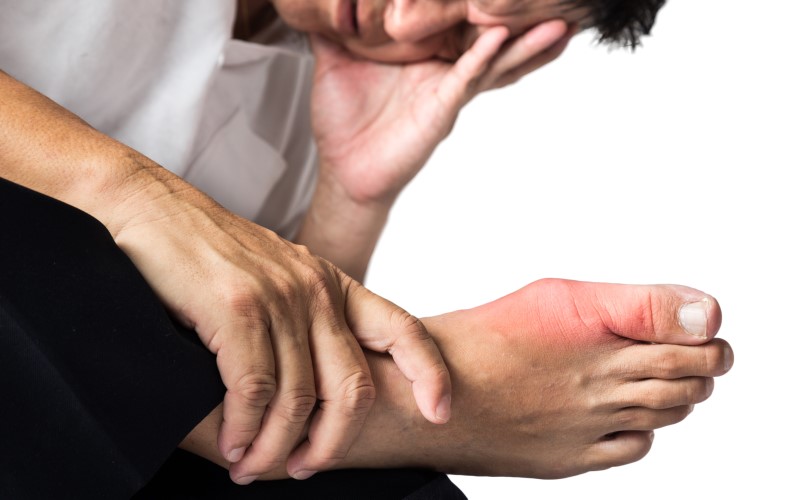
What is gout and what causes it?
Gout is a crystal arthritis that is very inflammatory. It is caused when a food protein called purine breaks down into urate. This is a normal part of metabolism, but for some people, it can result in too much urate in the blood. Depending on your genetics and other risk factors, high levels of urate can cause crystals to form in joints. When this happens, or if the urate levels continue to vary, this can cause inflammation around the crystals.
What are the symptoms of gout?
Gout usually starts as a very inflammatory arthritis, often in the limbs of the lower body and usually one joint at a time. The first time people experience gout, almost 50% will suffer the symptoms in their big toe. Most people who have gout once will have another gout attack within the first two years and it can increase over time, eventually affecting several joints. Joints furthest from the spine (hands, wrists, elbows, knees, ankles, feet) tend to be the most affected.
How is gout diagnosed?
During the early stages of gout, a flare tends to happen very suddenly. Flares tend to occur in evening, nighttime or morning and they come on very quickly–within the course of a few hours. There are several ways to diagnose gout, but the easiest time to diagnose it is when a person is having a joint flare. At this time, a provider is able to remove and analyze fluid from that joint to find whether there are crystals present.
Labs, symptoms and imaging are other ways to diagnose gout. If a person is in between flares, a blood test works well to determine the amount of uric acid in the blood. If a person has a history of repeated single joint flare, and during a time of non-flare they have highly elevated uric acid, it can be assumed they probably have gout. Ultrasound is highly sensitive for early gout and is a better treatment choice for trying to determine if a person has gout during a non-flare time. X-rays can be helpful if joint damage from gout has already taken place. Also, whether or not people get treatment in the beginning, flares tend to resolve on their own within a few hours or few days. If someone goes untreated for several years and has multiple flares, it can become more of a chronic arthritis where people have more chronic joint pain and inflamed joints.
How is gout treated?
Treatment for gout is geared toward getting inflammation under control. An anti-inflammatory NSAID, a corticosteroid medication, or a gout-specific medication will help control the inflammation. If you see a provider who is comfortable removing fluid, they can help get a good diagnosis right away and inject steroid directly into the joint, in some cases producing a faster resolution of symptoms compared to treatment with oral medication. Long-term treatment is geared towards reducing the uric acid and crystal burden over time. Your provider will monitor medications over time with blood tests looking at uric acid levels.
What are some ways to reduce the risk of having gout?
There are some reports that cherries or cherry juice can reduce gout flares. While this does not replace prescription medication for gout, some evidence that 12 cherries once or twice per day can reduce flares. There is some evidence that vitamin C and fish oil supplements may reduce flares.
What are the complications of gout?
In addition to swollen and painful joints, gout can cause long-term complications including damage to the joints and a large collection of uric acid crystals (so much so that it is visible–this is called tophi). Also, some patients may develop kidney stones and chronic kidney disease related to gout. Evidence suggests that having gout increases cardiovascular risk and treating gout with medications to lower uric acid can lower risk of stroke and heart attack.
If you have symptoms of gout, when should you seek care?
If a person has only had one gout attack, it’s usually worthwhile to wait and see if they’re going to have another attack. Some patients do not have more attacks, especially if they are able to modify their lifestyle choices. If you have had more than one gout attack, discuss this with your primary care provider so they can determine if some of the labs and tests are appropriate.
In the long-term, patients with gout should see a rheumatologist. There is good data that shows that patients who manage their gout with the help of a rheumatologist have better outcomes, less flares, have less joint damage, and are happier with their treatment outcome.
Bothered by gout and interested in an evaluation at the Rheumatology Clinic?
Please call Valley’s Rheumatology Clinic in Renton at 425.690.3495 or in Covington at 425.690.3494 for an appointment or visit valleymed.org/rheumatology.

